ESOPHAGUS-STOMACH-DUODENUM SURGERY Multiple Choice Questions :-
1. Which of the following statements about the anatomic course of the esophagus is correct?
A. The cervical esophagus passes behind and to the right of the trachea.
B. The thoracic esophagus enters the posterior mediastinum anterior to the aortic arch.
C. The thoracic esophagus passes behind the right mainstem bronchus and the pericardium.
D. The esophagus enters the diaphragmatic hiatus at the level of T8.
E. The esophagus deviates anteriorly and to the left as it enters the abdomen.
Answer: E
2. Which of the following statements about esophageal anatomy is correct?
A. The esophagus has a poor blood supply, which is segmental in distribution and accounts for the high incidence of anastomotic leakage.
B. The esophageal serosa consists of a thin layer of fibroareolar tissue.
C. The esophagus has two distinct muscle layers, an outer, longitudinal one and an inner, circular one, which are striated in the upper third and smooth in the distal two thirds.
D. Injury to the recurrent laryngeal nerve results in vocal cord dysfunction but does not affect swallowing.
E. The lymphatic drainage of the esophagus is relatively sparse, localized primarily to adjacent paraesophageal lymph nodes.
Answer: C
3. Which of the following statements about the lower esophageal sphincter (LES) mechanism, or high-pressure zone (HPZ), is true?
A. The LES is a circular smooth muscle ring that is 3 to 5 cm. long.
B. In assessing esophageal manometric data, mean HPZ pressure less than 6 mm. Hg or overall length less than 2 cm. is more likely to be associated with incompetence of the LES and gastroesophageal reflux.
C. Esophageal manometry and the acid perfusion (Bernstein) test reliably identify the patient with an incompetent LES mechanism.
D. Distal HPZ relaxation occurs within 5 to 8 seconds of initiating a swallow.
E. Twenty-four–hour distal esophageal pH monitoring is achieved with an intraesophageal pH electrode positioned at the esophagogastric junction.
Answer: B
4. Which of the following statements about esophageal motility is/are true?
A. The act of swallowing initiates UES relaxation, which persists until the bolus of food passes the LES.
B. The primary peristaltic wave normally propels the swallowed bolus through the esophagus in 4 to 8 seconds.
C. Normally, a progressive peristaltic contraction (primary wave) follows 50% of all swallows, the remainder being secondary or tertiary contractions.
D. Secondary peristalsis is initiated when the entire swallowed bolus of food fails to empty from the esophagus into the stomach.
E. Tertiary esophageal contractions are high-amplitude progressive peristaltic contractions that produce the “corkscrew” appearance of esophageal spasm on barium esophagography.
Answer: BD
5. Which of the following statements about UES dysfunction are correct?
A. This condition is diagnosed by the characteristic manometric findings of UES spasm.
B. Typical symptoms include cervical dysphagia, expectoration of saliva, and hoarseness.
C. The classic finding on barium esophagogram is a posterior cricopharyngeal bar.
D. Medical or surgical therapy of gastroesophageal reflux may be curative.
E. A cervical esophagomyotomy for UES dysfunction should be limited to 2 to 3 cm. in length so that normal muscle is not damaged.
Answer: BCD
6. Which of the following statements about achalasia is/are correct?
A. In most cases in North America the cause is a parasitic infestation by Trypanosoma cruzi.
B. Chest pain and regurgitation are the usual symptoms.
C. Distal-third esophageal adenocarcinomas may occur in as many as 20% of patients within 10 years of diagnosis.
D. Manometry demonstrates failure of LES relaxation on swallowing and absent or weak simultaneous contractions in the esophageal body after swallowing.
E. Endoscopic botulinum toxin injection of the LES, pneumatic dilatation, and esophagomyotomy provide highly effective curative therapy for achalasia.
Answer: D
7. Which of the following statements about diffuse esophageal spasm is/are true?
A. Chest pain due to esophageal spasm is readily differentiated from angina pectoris of cardiac origin.
B. Bouts of esophageal obstruction and regurgitation of food are characteristic.
C. Associated psychiatric disorders are common.
D. During manometric assessment, unless the patient is having pain there may be no detectable multiphasic, high-amplitude, simultaneous esophageal contractions.
E. The treatment of choice is a long esophagomyotomy from the aortic arch to the esophagogastric junction.
Answer: CD
8. Which of the following statements about epiphrenic diverticula of the esophagus is/are correct?
A. They are traction diverticula that arise close to the tracheobronchial tree.
B. They characteristically arise proximal to an esophageal reflux stricture.
C. The degree of dysphagia correlates with the size of the pouch.
D. They are best approached surgically through a right thoracotomy.
E. The operation of choice is a stapled diverticulectomy, long esophagomyotomy, and partial fundoplication.
Answer: E
9. Which of the following statements about Schatzki’s ring is correct?
A. The ring represents a panmural fibrotic stricture resulting from gastroesophageal reflux.
B. Dysphagia occurs when the ring diameter is 13 mm. or less.
C. The ring occurs within 1 to 2 cm. of the squamocolumnar epithelial junction.
D. Schatzki’s ring indicates reflux esophagitis.
E. Schatzki’s ring signifies the need for an antireflux operation.
Answer: B
10. Choose the distance in centimeters from the upper incisor teeth at which the following radiographically identified esophageal lesions would be encountered endoscopically:
A. 10 cm. 1. Zenker’s diverticulum
B. 15 cm. 2. Traction diverticulum
C. 25 cm. 3. Tumor 10 cm. proximal to the esophagogastric junction
D. 30 cm.
E. 40 cm.
Answer: 1-B, 2-C, 3-D
11. Which of the following statements about pathology encountered at esophagoscopy is/are correct?
A. Reflux esophagitis should be graded as mild, moderate, or severe, to promote consistency among different observers.
B. An esophageal reflux stricture with a 2-mm. lumen is not dilatable and is best treated with resection.
C. A newly diagnosed radiographic distal esophageal stricture warrants dilation and antireflux medical therapy.
D. In patients with Barrett’s mucosa, the squamocolumnar epithelial junction occurs 3 cm. or more proximal to the anatomic esophagogastric junction.
E. After fasting at least 12 hours, a patient with megaesophagus of achalasia can safely undergo flexible fiberoptic esophagoscopy.
Answer: D
12. Which of the following statements about the diagnosis and treatment of esophageal leiomyomas is/are correct?
A. The majority are diagnosed after they cause dysphagia and chest pain.
B. Biopsy is indicated at the time of esophagoscopy, to rule out carcinoma.
C. Full-thickness elliptical excision of the esophageal wall is the preferred surgical approach.
D. Endoscopic ultrasonography is a reliable means of following leiomyomas conservatively.
E. Recurrence of resected leiomyomas is minimized by wide local excision.
Answer: D
13. Which of the following statements regarding the pathology of esophageal carcinoma is/are correct?
A. Worldwide, adenocarcinoma is the most common esophageal malignancy.
B. Squamous cell carcinoma is most common in the distal esophagus, whereas adenocarcinoma predominates in the middle third.
C. Patients with Barrett’s metaplasia are 40 times more likely than the general population to develop adenocarcinoma.
D. Metastases from esophageal carcinoma are characteristically localized to regional mediastinal lymph nodes adjacent to the tumor.
E. Achalasia, radiation esophagitis, caustic esophageal stricture, Barrett’s mucosa, and Plummer-Vinson syndrome are all premalignant esophageal lesions that predispose to the development of squamous cell carcinoma.
Answer: C
14. Which of the following statements about the surgical treatment of esophageal carcinoma is/are correct?
A. The finding of severe dysphagia in association with Barrett’s mucosa is an indication for an antireflux operation to prevent subsequent development of carcinoma.
B. Long-term survival is improved by radical en bloc resection of the esophagus with its contained tumor, adjacent mediastinal tissues, and regional lymph nodes.
C. The morbidity and mortality rates for cervical esophagogastric anastomotic leak are substantially less than those associated with intrathoracic esophagogastric anastomotic leak.
D. The leading complications of transthoracic esophagectomy and intrathoracic esophagogastric anastomosis are bleeding and wound infection.
E. Transhiatal esophagectomy without thoracotomy achieves better long-term survival than transthoracic esophagectomy.
Answer: C
15. The best management for a 48-hour-old distal esophageal perforation is:
A. Antibiotics and drainage.
B. Division of the esophagus and exclusion of the perforation.
C. Primary repair with buttressing.
D. Resection with cervical esophagostomy, gastrostomy, and jejunostomy.
E. T-tube fistula and drainage.
Answer: C
16. A 50-year-old patient develops sudden left lower chest pain and epigastric pain after vomiting. The patient shows diaphoresis, breath sounds are decreased on the left, and there is abdominal guarding. The most appropriate diagnostic test is:
A. Aortography.
B. Esophagoscopy.
C. Electrocardiogram.
D. Film of the chest.
E. White blood count.
Answer: D
17. The following statements about the influence of diet and lifestyle on lower esophageal sphincter (LES) function are true except one. Identify the incorrect statement.
A. A high-protein diet increases LES pressure.
B. A fat meal results in sustained decrease in LES pressure.
C. Chocolate ingestion causes a decrease in LES pressure.
D. Peppermint produces a transient decrease in LES values.
E. Cigarette smoking produces no significant changes in LES pressures.
Answer: E
18. When a stricture is present in association with gastroesophageal reflux, each of the following is an acceptable repair for reflux control except one. Identify the poorest repair.
A. Intrathoracic total fundoplication.
B. Lengthening gastroplasty with total fundoplication.
C. Total fundoplication.
D. Lengthening gastroplasty with partial fundoplication.
E. Partial fundoplication.
Answer: E
19. When assessing gastroesophageal reflux disease by manometry each of the following statements is correct except one. Identify the incorrect one.
A. Absent or extremely low LES pressures have predictive value in identifying more severe reflux.
B. Peristaltic dysfunction increases with increasing severity of esophagitis.
C. With established reflux disease the UES is hypertensive.
D. Esophageal functional changes are worst in patients with a circumferential columnar-lined esophagus.
E. Absence of peristalsis may be associated with more severe forms of reflux disease.
Answer: C
20. The presence of a nonmalignant mid- or upper esophageal stricture always indicates the presence of:
A. Alkaline reflux esophagitis.
B. Barrett’s esophagus.
C. Idiopathic reflux disease.
D. Mediastinal fibrosis.
E. Scleroderma.
Answer: B
21. Which of the following is most reliable for confirming the occurrence of a significant esophageal caustic injury?
A. History of the event.
B. Physical examination of the patient.
C. Barium esophagraphy.
D. Endoscopy.
Answer: D
22. Indications for surgical reconstruction of the esophagus include which of the following?
A. Continuing requirement for frequent dilation of an extensive esophageal stricture for a minimum of 2 years.
B. Failure or refusal of the patient to comply with a treatment regimen of regular dilation.
C. Development of a fistula between the esophagus and tracheobronchial tree.
D. Iatrogenic perforation of the esophagus during attempted dilation.
Answer: BCD
23. First-line therapy for routine peptic duodenal ulcer disease includes:
A. Vagotomy and antrectomy.
B. Upper endoscopy and biopsy to rule out tumor.
C. Evaluation for Helicobacter pylori.
D. Serum gastrin determination.
E. Cream or milk-based “Sippy” diet.
Answer: C
24. Appropriate management of severe vomiting associated with gastric outlet obstruction from peptic ulcer disease includes all of the following except:
A. Nasogastric suction.
B. Intravenous hydration.
C. Nutritional assessment; upper endoscopy to rule out malignancy.
D. Intravenous H 2 antagonist.
E. Oral antacid therapy.
Answer: E
25. All of the following are complications of peptic ulcer surgery except:
A. Duodenal stump blowout.
B. Dumping.
C. Diarrhea.
D. Delayed gastric emptying.
E. Steatorrhea.
Answer: E
26. The presentation of Zollinger-Ellison syndrome includes all of the following except:
A. Hyperparathyroidism in patients with multiple endocrine neoplasia type 1 (MEN 1) syndrome.
B. Diarrhea.
C. Migratory rash.
D. Jejunal ulcers.
E. Duodenal ulcers.
Answer: C
27. All are true about the dumping syndrome except:
A. Symptoms can be controlled with a somatostatin analog.
B. Diarrhea is always part of the dumping syndrome.
C. Flushing and tachycardia are common features of the syndrome.
D. Separating solids and liquids in the patient’s oral intake alleviates some of the symptoms of the syndrome.
E. Early postoperative dumping after vagotomy often resolves spontaneously.
Answer: B
28. In patients with bleeding duodenal ulcers, the endoscopic finding associated with the highest incidence of rebleeding is:
A. Visible vessel.
B. Cherry-red spot.
C. Clean ulcer bed.
D. Duodenitis.
E. Shallow, 3-mm. ulcer.
Answer: A
29. All of the following are contraindications for highly selective vagotomy except:
A. Intractable duodenal ulcer disease.
B. Peptic ulcer disease causing gastric outlet obstruction.
C. Fundic peptic ulceration.
D. Cigarette chain smoking.
E. Perforated peptic ulcer disease with more than 24 hours’ soilage.
Answer: A
30. All the following are true of omeprazole except:
B. It works by blocking the hydrogen-potassium ATPase in the parietal cell.
C. It is parietal cell specific.
D. It has a short half-life (about 90 minutes) when taken orally.
E. It has been associated with gastric neoplasm in a rat model.
Answer: D
31. All of the following statements about gastrin-releasing peptide (GRP) are true except:
A. In species other than man and dog GRP is commonly referred to as bombesin.
B. GRP serves as a neurotransmitter.
C. GRP inhibits pancreatic secretion when given intravenously.
D. GRP stimulates gastric acid secretion when given intravenously.
E. GRP is released in response to cholinergic stimulation of the parietal cells to stimulate release of gastrin.
Answer: C
32. Cholecystokinin (CCK) is believed to function in all of the following processes except:
A. It physiologically delays gastric emptying.
B. It appears to have a role in satiety regulation.
C. It contracts the gallbladder.
D. It stimulates pancreatic secretion.
E. It is important in the control of the anal sphincter.
Answer: E
33. All of the following measures have been recommended for control of acid secretion in patients with Zollinger-Ellison syndrome except:
A. Antrectomy.
B. Highly selective vagotomy.
C. Total gastrectomy.
D. Vagotomy and pyloroplasty.
E. Medical therapy with Prilosec (omeprazole).
Answer: A
34. All of the following contribute to peptic ulcer disease except:
A. Cigarette smoking.
C. Helicobacter pylori.
D. Gastrinoma.
E. Spicy foods.
Answer: E
35. Which of the following statements about gastric polyps is/are true?
A. Like their colonic counterparts, gastric epithelial polyps are common tumors.
B. They are analogous to colorectal polyps in natural history.
C. Endoscopy can uniformly predict the histology of a polyp based on location and appearance.
D. In a given patient, multiple polyps are generally of a single histologic type.
E. Gastric adenomatous polyps greater than 2 cm. in diameter should be excised because of the risk of malignant transformation.
Answer: DE
36. Which of the following statements about gastric leiomyomas is/are true?
A. They are the most common type of gastric tumor of the stomach at autopsy.
B. The leiomyoblastoma cell type reflects malignant transformation of gastric leiomyomas.
C. A conservative surgical approach is indicated for their resection since regional lymphadenectomy has not been proved reliable even when they turn out to be malignant.
D. Severe hemorrhage may occur from deep ulcerations overlying the intramural tumor.
Answer: ACD
37. The sine qua non of the histologic diagnosis of a gastric pseudolymphoma is:
A. Extragastric extension of the gastric lesion.
B. Nodal involvement beyond the immediate stomach.
C. A germinal center in the gastric lesion.
D. Extension into esophagus and duodenum.
E. Unresponsive to conservative gastric resection.
Answer: C
38. All of the following statements about surgical management of gastric lymphomas are true except:
A. Stage I gastric lymphomas (small lesions confined to the stomach wall) can be cured completely with surgical therapy alone.
B. Extensive gastric lymphomas that initially are treated with radiation and/or chemotherapy occasionally perforate during treatment and require secondary resection.
C. Patients explored with a presumptive diagnosis of gastric lymphoma should undergo an attempt at curative resection when this is safe and feasible.
D. Without a preoperative diagnosis resection for gastric mass should not be attempted unless lymphoma can be excluded.
E. Appropriate staging for primary gastric lymphoma includes bone marrow biopsy.
Answer: D
39. Which of the following risk factors have been shown to increase significantly the incidence of gastrointestinal bleeding from stress gastritis in intensive care unit (ICU) patients?
A. Glucocorticoid administration.
B. Respiratory failure.
C. Coagulopathy.
D. Organ transplantation.
E. Jaundice.
Answer: BC
40. Which of the following measures are effective in preventing stress gastritis bleeding in critically ill patients?
A. Improving systemic circulation by correcting any shocklike state resulting from blood loss or sepsis.
B. Correcting systemic acid-base abnormality.
C. Maintaining adequate nutrition.
D. Reducing intragastric acidity by either antacid titration or H 2 antagonists.
Answer: ABCD
41. Which of the following have been used successfully to treat patients with vascular compression of the duodenum?
A. Subtotal gastrectomy and Roux-en-Y gastrojejunostomy.
B. Total parenteral nutrition.
C. Division of the ligament of Treitz and duodenal mobilization.
D. Percutaneous endoscopic gastrostomy.
E. Duodenojejunostomy.
Answer: BCE
42. Which of the following statements about the anatomic basis for the syndrome of vascular compression of the duodenum are true?
A. The duodenum is obstructed in its distal third as it crosses over the lumbar vertebral column.
B. Structures crossing beneath the superior mesenteric artery include the duodenum, the uncinate process of the pancreas, and the left renal vein.
C. Hyperextension of the back allows the angle of origin of the superior mesenteric artery to widen, lessening the obstruction of the duodenum.
D. Patients are at significant risk for vascular compression of the duodenum if the angle between the takeoff of the superior mesenteric artery and the aorta is less than 45 degrees.
E. Arteriographic studies show a typical area of extrinsic compression and narrowing of the arterial lumen due to duodenal pressure.
Answer: AB
43. Numerous epidemiologic associations have been made between (1) environmental and dietary factors and (2) the incidence of gastric cancer, including all except:
A. Dietary nitrites.
B. Dietary salt.
C. Helicobacter pylori infection.
D. Dietary ascorbic acid.
Answer: D
44. All of the following benign conditions are associated with increased rates of gastric cancer except:
A. Pernicious anemia.
B. Multiple endocrine neoplasia type I (MEN 1).
C. Adenomatous polyps.
D. Chronic atrophic gastritis.
Answer: B
45. Which of the following statements concerning the pathology of gastric cancer is true?
A. Distal gastric cancers are becoming more common.
B. Intestinal-type gastric tumors resemble colon carcinomas and have a better prognosis than diffuse type.
C. Early gastric cancers are confined to the mucosa and are lymph node negative.
D. Broders’ histologic grading system correlates well with survival: patients with grade IV tumors have 5-year survival rates around 65%.
Answer: B
46. An 80% distal gastrectomy is performed for a 6-cm. antral cancer with extension to the muscularis propria and three positive lymph nodes less than 3 cm. from the tumor. The stage of this tumor was:
A. Stage I.
B. Stage II.
C. Stage III A.
D. Stage III B.
Answer: B
47. Which of the following statements about the surgical treatment of gastric cancer is false?
A. Patients with tumors of the middle and proximal thirds should undergo total gastrectomy.
B. Adenocarcinoma of the cardia-gastroesophageal junction may require reconstruction in the abdomen, chest, or neck.
C. Palliative resection yields better results than palliative bypass.
D. Japanese patients who undergo gastric resection are, on average, 10 years younger and much leaner than their Western counterparts.
Answer: A
48. Which of the following measures of obesity correlates best with mortality?
A. The 1983 Metropolitan Life Insurance Company tables for ideal body weight.
B. Hydroimmersion measurements of body fat composition.
C. Body mass index (BMI).
D. Skinfold thickness.
E. Waist to hip ratios (WHR).
Answer: C
49. The most effective therapy for morbid obesity, in terms of weight control, is:
A. Intensive dieting with behavior modification.
C. A gastric bypass with a 40-ml. pouch, a 10- to 20-cm. Roux-en-Y gastroenterostomy.
D. A gastric bypass with a 15-ml. pouch, a 40- to 60-cm. Roux-en-Y gastroenterostomy.
E. Daily exercise with strong emphasis on utilizing all four limbs.
Answer: D
50. Which of the following statements about intestinal bypass is/are correct?
A. The operation produced weight loss similar to that of the gastric bypass.
B. The operation produced severe metabolic disturbances, including hypocalcemia, increased bile salts and glycine synthesis.
C. Bacterial overgrowth in the bypassed segment led to liver failure.
D. The operation demonstrated that an adult human could survive with 40 to 50 cm. of small intestine.
Answer: ABCD
51. Which of the following is/are contraindications to gastric bypass surgery?
A. Diabetes mellitus.
B. Hypertension.
C. Pickwickian syndrome.
D. Failure to agree to long-term follow-up.
E. Sleep apnea.
Answer: D
52. A 34-year-old morbidly obese diabetic woman underwent a gastric bypass about 12 hours ago. The operation was technically difficult but finally went well. You are called because she now has a temperature of 99.2? F, pulse of 134, and some pain in her incision and her back. She looks well; the incision is clean; and her examination is otherwise negative. A bolus of 500 ml. of dextrose/lactated Ringer’s did not change her vital signs, except that her pulse rose to 140 without an increase in urine output. Your next step should be:
A. Another bolus of crystalloids.
B. Posterioanterior and lateral chest films.
C. Obtain white cell count, differential count, and electrolyte values.
D. Call the operating room and warn them that you need to re-explore for a leak.
E. Increase her pain medication.
Answer: D
53. Metabolic complications of subtotal gastrectomy with Billroth I or Billroth II reconstruction include:
A. Hypothyroidism.
B. Anemia.
C. Reactive hypoglycemia.
D. Dumping syndrome.
E. Metabolic bone disease.
Answer: BCDE
54. Which of the following statement(s) concerning the surgical options for an anti-reflux operation is/are true?
a. A patient with normal esophageal length and esophageal body motility is best served by laparoscopic Nissen fundoplication
b. A patient with a low peristaltic amplitude of the distal third of the esophagus is a candidate for an open Nissen fundoplication
c. A Collis gastroplasty is an additional procedure that can be added in patients with extensive esophageal shortening
d. End-stage reflux disease such as an undilatable stricture or Barrett’s esophagus with high grade dysplagia is best managed by a colon interposition
Answer: a, c, d
55. Factors associated with the development of complications of gastroesophageal reflux disease include:
a. The presence of a defective lower esophageal sphincter
b. Inadequate esophageal clearance
c. The presence of a hiatal hernia
d. The presence of an alkaline component of the reflux material
Answer: a, b, c, d
56. Fundamental to understanding disorders of esophageal function is the measurement of the contractility of the esophageal body and sphincters. Which of the following statement(s) is/are true concerning esophageal manometry in the investigation of benign esophageal disease?
a. A defective sphincter is predictive of poor long-term response to medical therapy, but a good response to surgery
b. Esophageal manometry can determine the resting pressure and the overall length of the sphincter but not its abdominal length
c. The LES pressure normally drops to gastric baseline immediately after a swallow before the peristaltic wave reaches the lower esophagus
d. A Vector Volume below the fifth percentile of normal is the most sensitive measure of mechanical deficiency of the LES
e. There is no correlation between defects in LES with the severity of gastroesophageal reflux disease
Answer: a, c, d
57. Which of the following statement(s) is/are true concerning the diagnosis and management of the patient whose barium esophogram is shown in Figure 18-29?
a. The condition is due to neuronal generation of the myenteric plexus in the lower esophageal sphincter
b. The patient will report symptoms of vomiting of sour or bitter material
c. Despite the impressive radiologic picture, passage of the endoscope through the area of narrowing will likely be possible
d. Manometry and 24 hour pH monitoring should be performed for confirmation of the diagnosis
Answer: c
58. Which of the following statement(s) is/are true concerning other tests available for investigation of esophageal disease?
a. A 24 hour pH monitoring is currently the principal method in making the diagnosis of gastroesophageal reflux disease (GERD)
b. Acid reflux episodes are defined as periods when the esophageal pH is less than 2
c. Twenty-four pH monitoring is only useful in the detection of acid reflux disease
d. The Bernstein test continues to be an important tool in the diagnosis of acid reflux disease
e. Delayed gastric emptying may be an important etiologic factor in patients with GERD
Answer: a, e
59. The results for anti-reflux surgery are generally good, however, patients who have failed anti-reflux procedures constitute a particularly challenging group. Which of the following statement(s) is/are true concerning failed anti-reflux repairs?
a. A Slipped Nissen is usually the result of an operative technical mistake
b. Disruption of a fundoplication is more prone to occur with a Nissen fundoplication because of the use of the gastric wall in the repair
c. Postoperative dysphagia in a patient with normal preoperative motility is usually due to a secondary motility disorder
d. Colonic replacement, although technically challenging, usually has superior long-term results when compared to esophageal replacement with the stomach
Answer: a, d
60. A number of diagnostic modalities exist for investigation of structural abnormalities of the esophagus. Which of the following statement(s) is/are true concerning the use of these investigative studies?
a. Endoscopy should be the first investigation in any patient with foregut symptoms
b. Barrett’s esophagus is suggested when the squamo-columnar junction is more than 2 cm above the gastroesophageal junction on endoscopic examination
c. There are three areas of esophageal narrowing which can be noted on both barium esophogram and endoscopy
d. The CT appearance of the esophagus is normally a flattened, hollow structure with a thin wall
Answer: b, c, d
ESOPHAGUS-STOMACH-DUODENUM SURGERY Objective type Questions with Answers
61. Which of the following patient scenarios would be best managed with anti-reflux surgery?
a. A patient with heartburn but normal 24 hour pH monitoring and an intact lower esophageal sphincter
b. A patient with primarily respiratory manifestations of gastroesophageal reflux
c. A patient with increased acid exposure and a mechanically defective sphincter who responds well to medical therapy but requires continued long-term medication for continued relief
d. A patient with gastroesophageal reflux but excessive complaints of epigastric pain, nausea, vomiting, and loss of appetite
Answer: b, c
62. Which of the following statement(s) concerning pharyngoesophageal disorders is/are true?
a. In neuromuscular diseases, dysphagia is often worse for liquids than for solids
b. Cricomyotomy may be indicated for a wide variety of neuromuscular disorders involving the pharyngoesophageal phase of swallowing
c. Excision of a Zenker’s diverticulum is indicated to prevent malignant change in the sac
d. Complications of all operations on the cervical esophagus include hematoma formation and recurrent nerve paralysis
Answer: a, b, d
63. Barrett’s esophagus is a complication of gastroesophageal reflux disease. Which of the following statement(s) is/are true concerning this condition?
a. The histologic hallmark is the presence of “specialized” columnar epithelium regardless of how far it extends into the esophagus
b. Barrett’s epithelium will frequently regress with medical therapy or anti-reflux surgery
c. High grade dysplasia will frequently be associated with foci of invasive carcinoma
d. Patients with adenocarcinoma arising in Barrett’s esophagus have a high incidence of p53 gene mutations
Answer: a, c, d
64. Which of the following statement(s) is/are true concerning the blood supply and lymphatic drainage of the esophagus?
a. The thoracic esophagus receives no direct branches from the aorta therefore allowing the technique of transhiatal (blunt) esophagectomy
b. Bleeding esophageal varices are most prominent in the mid-esophagus
c. Lymphatic drainage of the lower third of the esophagus goes entirely to the abdominal lymphatic system
d. Nodal involvement in esophageal cancer is quite common even if the tumor is limited to the level of the submucosa
Answer: d
65. Which of the following statement(s) is/are true concerning the process of swallowing and esophageal transit of food?
a. Injury to the recurrent laryngeal nerves can cause motility problems of the cervical esophagus and resulting aspiration
b. Esophageal reflux does not lead to impaired esophageal motility
c. Relaxation of the LES is mediated via inhibitory neurons
d. The overall length of the LES is the only factor influencing the pressure gradient of the sphincter
e. A mechanically defective sphincter is always associated with increased esophageal acid exposure
Answer: a, c
66. Which of the following statement(s) is/are true concerning the management of this patient?
a. The risk of perforation of the esophagus associated with balloon dilatation may be as high as 10%
b. An anti-reflux procedure should be universally performed for any operative myotomy
c. Successful relief of dysphagia can be achieved in up to 90% of patients with a single pneumatic dilatation
d. Thoracoscopic myotomy is associated with significantly poorer results than the open procedure
e. Prospective randomized studies and retrospective data appear to support a surgical approach for achalasia
Answer: a, e
67. Which of the following statement(s) is/are true concerning the surgical anatomy of the esophagus?
a. Surgical exposure of the cervical esophagus is best gained via the right neck
b. Spontaneous esophageal perforation tends to be associated with leakage into the left chest
c. Access to the entire thoracic esophagus can be obtained only via the left chest
d. The lower esophageal sphincter can be recognized distinctly by inspection of the gastroesophageal junction
Answer: b
68. Which of the following statement(s) is/are correct concerning the patient whose barium esophogram is shown below?
a. The patient’s complaint would be primarily chest pain and to a lesser degree dysphagia
b. The pathognomic feature of manometry is the presence of prolonged high amplitude waves
c. The patient will likely experience nutritional problems
d. The first line of treatment for this patient is surgical myotomy
Answer: a, b
69. Which of the following statement(s) is/are true concerning tracheoesophageal fistulas?
a. The majority of acquired tracheoesophageal fistulas are due to malignant disease
b. A water-soluble contrast esophogram should be obtained for diagnosis
c. Malignant tracheoesophageal fistulas represent one of the few indications for an endoesophageal prosthesis
d. A benign tracheoesophageal fistula from an endotracheal intubation injury often requires a thoracotomy for repair
Answer: a, c
70. Esophageal cysts arise as outpouchings of the embryonic foregut. Which of the following statement(s) is/are true concerning esophageal cysts?
a. The cyst lining will be lined only by stratified squamous epithelium
b. Most esophageal cysts cause symptoms in the first year of life
c. An asymptomatic esophageal cyst can be managed conservatively
d. The diagnosis of an esophageal cyst is usually made radiographically
Answer: b, d
71. Which of the following statement(s) is/are true concerning infectious esophagitis?
a. Candida albicans is not normally found in the mouth but results from the overgrowth of this fungus in patients on broad spectrum antibiotics
b. Candida esophagitis is usually self-limited and is seldom associated with chronic problems
c. Systemic therapy is seldom indicated
d. Small ulcers on barium esophogram in a transplant patient complaining of dysphagia and odynophagia are likely due to herpes simplex viral infection
Answer: d
72. Which of the following statement(s) is/are true concerning the pathology of squamous cell carcinoma of the esophagus?
a. Carcinoma in situ will gradually progress to invasive squamous cell carcinoma over a period of two to four years
b. The most common location for squamous cell carcinoma of the esophagus is the upper and mid-thoracic segment
c. Esophageal carcinoma tends to be multifocal
d. Macroscopically, ulcerative lesions with extensive infiltration of the adjacent esophageal wall are most common
e. Lymph node metastases are present in at least 75% of patients at the time of initial diagnosis
Answer: a, b, d, e
73. A 54-year-old woman experiences pain in both the anterior and posterior left chest and the epigastrium following balloon dilatation performed for achalasia. Which of the following statement(s) is/are true concerning this patient’s diagnosis and management?
a. A normal chest x-ray will rule out an esophageal perforation
b. Barium should never be used in performance of a contrast study with a diagnosis of esophageal perforation
c. Conservative, nonoperative treatment may be indicated
d. If surgical repair is necessary, the patient should undergo esophagomyotomy and a partial gastric fundoplication
Answer: c, d
74. Which of the following statement(s) is/are correct concerning the diagnostic studies for esophageal carcinoma?
a. A chest and upper abdominal CT scan is useful for both staging and predicting resectability
b. A barium swallow is an unnecessary test in a patient with dysphagia
c. Bronchoscopy should be performed in all patients with carcinoma of the upper and middle thirds of the esophagus
d. Bone and brain scans should be obtained routinely to rule out distant metastasis
e. Endoscopic ultrasound is a potentially sensitive examination for the staging of esophageal cancer
Answer: c, e
75. Which of the following conditions are associated with the development of esophageal carcinoma?
a. Caustic esophageal stricture
b. Achalasia of the esophagus
c. Plummer-Vinson syndrome
d. Esophageal diverticula
Answer: a, b, c, d
76. Which of the following statement(s) is/are correct concerning the options for resection of esophageal carcinoma?
a. The development of reflux esophagitis seldom occurs following intrathoracic resection due to the limited life expectancy of these patients
b. Transhiatal esophagectomy, although conceptually sound, is not technically possible in most patients with esophageal carcinoma
c. Transhiatal resection, although less morbid, has unfavorable survival statistics compared to transthoracic resection
d. Radical transthoracic esophagectomy with en bloc dissection of continuous lymph node bearing tissues has not been shown to improve survival over transhiatal esophagectomy
Answer: d
77. The incidence of adenocarcinoma of the esophagus is increasing at a very rapid rate, which is largely the result of the growing prevalence of adenocarcinoma arising in Barrett’s mucosa. Which of the following statement(s) is/are true concerning adenocarcinoma of the esophagus?
a. Barrett’s mucosa with specialized columnar epithelium characterized by veliform folds, lined by secreting columnar and goblet cells has the highest association with carcinoma of the esophagus
b. Less than 5% of patients with Barrett’s mucosa will harbor adenocarcinoma
c. Severe dysplasia of Barrett’s mucosa requires frequent reexamination and biopsy
d. Adenocarcinoma of the esophagus has a less aggressive behavior than squamous cell carcinoma
Answer: a
78. Which of the following statement(s) is/are true concerning esophageal diverticula?
a. A Zenker’s diverticulum characteristically occurs in older patients
b. Mediastinal granulomatous disease usually results in a mid-esophageal traction diverticulum which is usually asymptomatic
c. An epiphrenic diverticulum that presents to the right of the esophagus should be managed via left thoracotomy
d. Minimally symptomatic epiphrenic diverticula should not be operated upon
Answer: b, c, d
79. Which of the following statement(s) is/are true concerning caustic injury to the esophagus?
a. Alkaline injury is more destructive than acid injury
b. Acid ingestion is not injurious to the stomach due to its normal acidic pH
c. Ingested caustic agents rapidly pass through the esophagus and stomach into the small intestine
d. Unless perforation occurs, clinical manifestations resolve quickly with initial clinical improvement noted
e. Children are less likely to form a late esophageal stricture than adults
Answer: a, d, e
80. Which of the following statement(s) is/are true concerning nonresectional therapy for esophageal carcinoma?
a. Radiation therapy can be associated with five-year survival rates equal to surgery
b. Esophageal intubation to provide palliation for esophageal cancer is associated with minimal morbidity and mortality
c. Endoscopic laser fulguration is successful in up to 75% of patients
d. There is little or no role for surgical bypass for unresectable esophageal carcinoma
Answer: c, d
81. Benign tumors of the esophagus are rare constituting less than 1% of esophageal neoplasms. Which of the following statement(s) is/are true concerning benign esophageal neoplasms?
a. Most esophageal polyps are located just above the gastroesophageal junction
b. Malignant degeneration of leiomyomas of the esophagus is a frequent occurrence
c. An asymptomatic leiomyoma can be safely observed and followed with periodic barium esophograms and endoscopic ultrasonography
d. Most leiomyomas of the esophagus require esophagectomy
Answer: c
82. In an effort to improve survival following esophageal resection, trials of multi-modality therapy in combination with surgery have been completed. Which of the following statement(s) is/are true concerning such treatment?
a. Therapy appears to be indicated in squamous cell carcinoma but not adenocarcinoma
b. No residual carcinoma may be found in the resected specimen in up to 20% of patients
c. Nonrandomized trials would suggest improved survival compared to patients receiving surgery alone
d. Perioperative morbidity is increased due to preoperative radiation and chemotherapy
Answer: b, c,
83. Which of the following statement(s) is/are correct concerning the management of a patient with a caustic esophageal or gastric injury?
a. Corticosteroids should be administered immediately
b. Complete endoscopic examination of the esophagus and stomach should be completed
c. Patients requiring operative intervention are best explored through the abdomen
d. If organ resection is indicated, restoration of alimentary continuity should be deferred until the patient has recovered from the acute insult
e. In patients with esophageal stricture following second and third degree burns, dilatation therapy should be instituted as soon as possible after the injury
Answer: b, c, d
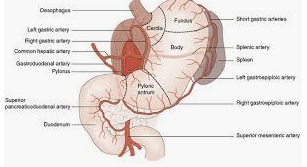
84. In regard to the arterial blood supply to the stomach, which of the following statement(s) is/are true?
a. The right gastric artery, a branch of the superior mesenteric artery, supplies the gastric antrum
b. Because of rich intramural collaterals, gastric viability may be preserved after ligation of all but one major artery
c. In cases of celiac artery occlusion, gastric viability is maintained collaterally via pancreaticoduodenal arcades
d. The left gastroepiploic artery is a branch of the celiac trunk
Answer: b, c
85. At a cellular level, the major stimulant(s) of acid secretion by the gastric parietal cell is/are:
a. Histamine
b. Prostaglandin E2
c. Acetylcholine
d. Gastrin
e. Norepinephrine
Answer: a, c, d
86. Which of the following statement(s) regarding the vagus nerves is/are true?
a. The right and left vagus nerves derive from a nerve plexus inferior to the tracheal bifurcation
b. The posterior vagus nerve is closely applied to the intrathoracic esophagus
c. The anterior vagus supplies a hepatic division which passes to the right in the lesser omentum
d. Approximately 90% of vagal fibers are afferent, transmitting information from the gastrointestinal tract to the central nervous system
e. The vagus nerves transmit gastroduodenal pain sensations associated with peptic ulceration
Answer: a, c, d
87. Important stimulants of gastrin release from endocrine cells in the antrum include:
a. Acidification of the antral lumen
b. Small peptide fragments and amino acids from luminal proteolysis
c. Locally released somatostatin
d. Dietary fats
Answer: b
88. Which of the following statements regarding human gastric acid secretion is/are true?
a. Fasting acid secretion, normally 2 to 5 mEq/h, is due to ambient vagal tone and histamine secretion
b. Truncal vagotomy decreases basal secretion by 80%
c. Histamine2 receptor antagonist administration can decrease basal acid secretion by 80%
d. Fasting acid secretion, normally 5 to 10 mEq/h, is due to circulating levels of gastrin
Answer: a, b, c
89. As a meal is emptied from the stomach, gastric acid secretion gradually returns to baseline. Which of the following statements correctly characterize control of gastric acid secretion?
a. In humans, the most important inhibitory influence on gastrin release is exposure of the gastric mucosa to luminal acid
b. Acidification of the antral lumen causes reciprocal increases in somatostatin release and decreases in gastrin secretion
c. Antral distension stimulates gastric acid secretion
d. Acidification of the duodenal bulb inhibits gastric acid secretion
e. Exposure of the duodenum to hyperosmolar solutions inhibits acid secretion
Answer: a, b, d, e
90. Which of the following statements correctly characterizes gastric motor activity associated with ingestion of a meal?
a. Ingested gastric volumes are accommodated with little increase in pressure by reflex relaxation of the proximal stomach
b. Receptive gastric accommodation is unaffected by proximal gastric vagotomy
c. In humans, liquid emptying occurs more quickly than solid emptying
d. Gastric emptying of liquids is not affected by proximal gastric vagotomy
Answer: a, c
91. It is widely agreed that the gastric mucosa secretes bicarbonate in addition to acid. Gastric secretion of bicarbonate is correctly characterized by which of the following statements?
a. Bicarbonate is secreted by chief cells within gastric crypts
b. Gastric bicarbonate secretion is stimulated by acetylcholine
c. Gastric bicarbonate secretion during fasting results in luminal pH above 6 in normal individuals
d. Prostaglandin E2 is a potent stimulant of gastric bicarbonate secretion
Answer: b, d
92. Gastric mucosal blood flow is regulated by neural, hormonal, and locally active influences. Which of the following statements correctly characterizes gastric blood flow?
a. Stimulation of sympathetic nerves supplying the stomach is followed by gastric mucosal hyperemia and increased total gastric blood flow
b. Vagal nerve stimulation is accompanied by decreased gastric mucosal blood flow
c. Stimulants that increase acid secretion increase mucosal blood flow
d. In humans, prostaglandins increase mucosal blood flow at doses that inhibit gastric acid secretion
Answer: c, d
93. Which of the following statements regarding intrinsic factor is/are correct?
a. Intrinsic factor is produced in chief cells located in the gastric fundus
b. Total gastrectomy is followed by folate deficiency due to vitamin malabsorption secondary to intrinsic factor deficiency
c. Intrinsic factor secretion, like that of acid, is stimulated by gastrin, histamine, and acetylcholine
d. Intrinsic factor deficiency accompanies H pylori-caused antral gastritis
Answer: c
94. A 24-year-old woman develops epigastric pain and has a diagnosis of duodenal ulcer confirmed by esophagogastroduodenoscopy. The patient is in the third month of a pregnancy. The most appropriate treatment would be:
a. Proximal gastric vagotomy
b. Misoprostol 400 mg b.i.d.
c. Sucralfate 1 gm q.i.d.
d. Cimetidine 400 mg b.i.d.
Answer: c
95. Helicoabacter pylori has been investigated as a possible etiologic agent in duodenal ulceration. Which of the following statement(s) regarding H pylori infection in humans is/are correct?
a. H pylori may be isolated from antral gastric mucosa in nearly 100% of patients with active duodenal ulceration but only 1–2% of normal volunteers
b. H pylori possess cell surface receptors that bind to small intestinal mucous cells
c. Therapeutic regimens for duodenal ulcer that eliminate the organism are associated with lower ulcer recurrence rates than those in which the organism persists
d. The incidence of the organism in the normal population increases with age
e. Antral gastritis is associated with development of duodenal ulcer
Answer: c, d, e
96. A 40-year-old male undergoes treatment of acute duodenal ulceration with cimetidine 400 mg b.i.d. and has resolution of symptoms by 6 weeks. The medication is continued as a nocturnal maintenance dose at the end of a three month treatment course. Recurrent symptoms develop 6 months after initial diagnosis and repeated endoscopic examination reveals recurrent ulceration. Biopsies of antral mucosa demonstrate moderate gastritis and the presence of H pylori. Medical management designed to eradicate H pylori and heal ulceration should include which of the following agents?
a. Cimetidine
b. Bismuth subcitrate
c. Amoxicillin
d. Metronidazole
e. Vancomycin
Answer: a, b, c, d
97. Development of duodenal ulceration is dependent upon gastric acid secretion. Which of the following statements correctly characterizes acid secretion in duodenal ulcer patients?
a. Groups of duodenal ulcer patients demonstrate decreased basal acid secretion
b. Maximal acid output to histamine averages 40 mEq/h in duodenal ulcer patients, twice that of normal
c. Tissue gastrin levels, on average, are twice normal in patients with active ulceration
d. Exogenously administered somatostatin is ineffective in suppressing acid secretion in patients with active ulceration
Answer: b
98. A 45-year-old man undergoes proximal gastric vagotomy for treatment of intractable duodenal ulceration. What physiologic alterations might be anticipated as a consequence of the operation?
a. Reduction of basal acid secretion by approximately 25%
b. Accelerated gastric emptying of liquids
c. Accelerated gastric emptying of solids
d. Fasting hypergastrinemia
e. Postprandial hyperinsulinemia
Answer: b, d
99. Which of the following statements regarding postoperative rates of recurrent ulcer and dumping is/are correct?
a. Truncal vagotomy and antrectomy is associated with persistent dumping in 10–15% of patients
b. Recurrent ulceration following truncal vagotomy and pyloroplasty is observed in 25% of patients within 10 years of operation
c. Patients that undergo proximal gastric vagotomy have a risk of recurrent ulcer of 10–15% and a risk of persistent dumping approximating 1%
d. Recurrent ulceration occurs in 5% of patients that undergo truncal vagotomy and antrectomy
Answer: a, c
100. Which of the following statement(s) is/are correct with regard to pyloric obstruction secondary to peptic ulceration?
a. Pyloric obstruction is suggested by hypochloremic hyponatremic alkalosis
b. Pyloric obstruction is suggested by hypochloremic hypokalemic alkalosis
c. Approximately 80% of patients with benign gastric outlet obstruction obtain permanent relief of symptoms by endoscopically-directed balloon dilatation
d. The lifetime risk of pyloric obstruction in peptic ulcer patients is 40%
Answer: b
101. A 42-year-old man with a recently diagnosed duodenal ulcer develops melena and near-syncope. After fluid resuscitation, upper gastrointestinal endoscopy is performed. During the examination, a 1 cm ulcer is noted in the proximal duodenum. A fresh clot is observed within the ulcer and blood is noted to be oozing around the clot. Optimal therapy would consist of which of the following?
a. Angiographic embolization of the gastroduodenal artery
b. Irrigation of the clot followed by endoscopic application of a heat probe
c. Transfusion and intravenous cimetidine
d. Angiographic infusion of vasopressin into the gastroduodenal artery
e. Transfusion and oral omeprazole
Answer: b
102. A 50-year-old patient has undergone truncal vagotomy and antrectomy with Billroth II reconstruction two years ago. The patient now complains of recurrent postprandial pain, nausea, and vomiting. Endoscopic examination reveals bile in the stomach; endoscopic biopsies demonstrate histologic evidence of moderately severe gastritis. No other endoscopic abnormalities are noted. Appropriate therapy could include:
a. Octreotide administration
b. Total gastrectomy
c. Conversion of Billroth II gastrojejunostomy to Billroth I gastroduodenostomy
d. Conversion of Billroth II gastrojejunostomy to Roux-en-Y gastrojejunostomy
e. Roux-en-Y hepaticojejunostomy
Answer: d
103. A 50-year-old male with a 2 year history of duodenal ulceration develops sudden, severe epigastric pain 4 hours prior to evaluation. Physical examination reveals T 101° F, pulse 80, BP 125/90, diminished bowel sounds, and abdominal muscular rigidity. An upright chest x-ray reveals pneumoperitoneum. At laparotomy, an anterior perforation in the first portion of the duodenum is observed. Optimal treatment would include:
a. Omental patch of the perforation followed by truncal vagotomy and antrectomy after 8 weeks
b. Omental patch of the perforation followed by truncal vagotomy and pyloroplasty after 8 weeks
c. Omental patch of the perforation followed by chronic cimetidine administration
d. Omental patch of the perforation plus proximal gastric vagotomy
e. Omental patch of the perforation only
Answer: d
104. Which of the following clinical circumstances have been identified as predisposing factors for the development of stress ulceration?
a. Intraperitoneal sepsis
b. Hemorrhagic shock
c. Isolated tibial fracture
d. 50% total surface area second degree burn
e. Adult respiratory distress syndrome
Answer: a, b, d, e
105. Type I gastric ulcers are located in the gastric body, usually along the lesser curvature. Which of the following statements correctly characterize type I gastric ulcers?
a. Normal to low acid secretion
b. Associated duodenal ulceration
c. High frequency of blood group A
d. Associated hypergastrinemia frequent
Answer: a, c
106. Which of the following statement(s) is/are correct regarding gastric ulcers greater than 3 cm in size?
a. Giant gastric ulcers occur in 30–40% of cases along the greater curvature
b. The risk of malignancy increases with increasing size of the ulcer
c. The treatment of choice for giant gastric ulcer is resection to include the ulcer
d. Giant gastric ulcer is a complication of intraarterial hepatic chemotherapy
Answer: b, c
107. With regard to benign gastric ulceration, the most common location of disease is which of the following?
a. Along the greater curvature
b. Immediately distal to the esophagogastric junction along the lesser curvature
c. In the area of the incisura angularis along the lesser curvature
d. Within the gastric antrum
Answer: c
108. Which of the following statement(s) regarding gastric mucosal defense is/are correct?
a. Gastric mucus, produced by the surface epithelial cells, forms an unstirred layer over the gastric surface
b. Gastric parietal cells produce a bicarbonate-rich fluid
d. Gastric mucus provides substantial buffering capacity that maintains near-neutrality near the epithelial surface
Answer: a
109. A 35-year-old smoker is involved in a house fire and receives a 45% total surface area burn. One half of the burned surface appears to be third degree. On the third post-burn day, the patient is noted to have bloody drainage from a nasogastric tube and a decrease of 5% in his hematocrit. Appropriate management should include which of the following?
a. Urgent upper gastrointestinal contrast study to delineate site of bleeding
b. Immediate selective arteriography via the left gastric artery to diagnose and treat presumed stress ulceration
c. Urgent esophagogastroduodenoscopy to diagnosis the cause of bleeding
d. Urgent intravenous infusion of vasopressin at 0.2–0.4 IU/min
Answer: c
110. Agents demonstrated to have an efficacy of greater than 90% for prophylactic treatment of stress ulceration include which of the following?
a. Antacids
b. H2 receptor antagonists
c. Sucralfate
d. Misoprostil
Answer: a, b, c
111. A 45-year-old male presents with symptoms of epigastric pain, worsened with ingestion of food. Physical examination is normal. Upper abdominal ultrasonography is unremarkable. Contrast radiography reveals a 2 cm ulcer in the gastric fundus along the lesser curvature. Therapy with omeprazole 20 mg per day is begun but symptoms persist 3 weeks later. Appropriate management includes which of the following?
a. Increase in omeprazole dose to 40 mg per day
b. Addition of sucralfate 1 gm every 8 hours
c. Addition of cimetidine 200 mg b.i.d.
d. Esophagogastroduodenoscopy with biopsy of ulceration
Answer: d
112. A 52-year-old woman is hospitalized with acute upper gastrointestinal hemorrhage. Endoscopic examination reveal a 2.5 cm ulcer in the area of the incisura angularis. The remainder of the endoscopic examination is normal. Continued bleeding requires operative therapy. Optimal therapy consists of which of the following?
a. Gastrotomy with oversewing of the bleeding site
b. Distal gastrectomy including the area of ulceration
c. Proximal gastric vagotomy and oversewing of the bleeding ulcer
d. Truncal vagotomy, pyloroplasty, and oversewing of the bleeding ulcer
Answer: b
113. A 25-year-old man is involved in an automobile accident with resultant injuries including bilateral closed femur fractures, left pulmonary contusion, and closed head injury. On post-injury day 4, significant upper gastrointestinal hemorrhage begins. Endoscopic examination reveals an area of confluent ulceration with bleeding in the gastric fundus. Endoscopic hemostasis fails. Appropriate immediate management includes:
a. Lavage of gastric contents with iced saline
b. Urgent total gastrectomy
c. Selective arterial infusion of vasopressin via the left gastric artery
d. Insertion of Sangstaken-Blakemore balloon
Answer: c
114. Which of the following statements regarding gastroplasty and gastric bypass for morbid obesity is/are correct?
a. Horizontal gastroplasty techniques that rely on a single horizontal application of a stapling device are associated with weight loss “failure” rates of 40% to 70%
b. Gastric bypass is followed by progressive weight loss over a period of 36 months
c. Gastric bypass is associated with a “failure” of weight loss in 10 to 15% of patients
d. With three superimposed applications of a stapling device, gastric bypass staple line dehiscence occurs in less than 2%
Answer: a, c, d
115. Severe obesity is associated with a large number of associated problems that form the basis of the term morbid obesity. Documented causes of excess mortality in severely obese patients include:
a. Coronary artery disease
b. Hypertension
c. Adult-onset diabetes mellitus
d. Obesity hypoventilation and sleep apnea
e. Pulmonary embolization
Answer: a, b, c, d, e
116. Jejunoileal bypass was formerly performed as a weight reduction procedure. The operation has now been abandoned due to the development of serious long-term complications associated with the procedure. Which of the following statements correctly characterize results following jejunoileal bypass?
a. Kidney stones occur with increased frequency due to increased absorption of pyruvate from the colon
b. The most serious complication of jejunoileal bypass is development of cirrhosis due to protein calorie malnutrition
c. Bacterial overgrowth in the bypassed segment can be treated with oral vancomycin
d. Rapid weight loss following jejunoileal bypass is associated with development of gallstones
Answer: b, d
117. Which of the following statements is correct with regard to gastric bypass for obesity?
a. Rapid weight loss following successful gastric bypass for obesity is associated with an increased risk of developing cholelithiasis
b. Marginal ulcer develops in 25% of gastric bypass patients
c. Vitamin B12 deficiency is a potential complication of gastric bypass due to gastric mucosal atrophy
d. Anastamotic leak after gastric bypass is often heralded by bradycardia
Answer: a
118. With regard to operative treatment of gastric carcinoma, which of the following statements is/are correct?
a. Resectional margins of 2 cm are necessary to prevent recurrence due to intramural metastases
b. Prophylactic splenectomy has been shown to improve outcome in similarly staged patients
c. Extended lymphadenectomy including nodes along the aorta and esophagus has not been shown to improve survival in North American trials
d. Long-term survival is rare if adjacent organs must be resected to achieve local control
Answer: c, d
119. Which of the following statement(s) characterizing gastric lymphoma is/are correct?
a. More than half of gastrointestinal lymphomas occur in the stomach
b. The peak incidence of gastric lymphoma is in the 2nd and 3rd decade
c. Endoscopic biopsy is positive diagnostically in 90% of cases
d. Gastric perforation occurs in 40% of patients treated with cytolytic agents instead of gastrectomy
Answer: a, c
120. A patient with gastric adenocarcinoma undergoes subtotal gastrectomy. Pathological examination reveals that the tumor penetrates to the serosa. Regional lymph nodes are not involved. Distant metastases are not detected. What is the correct tumor stage and 5-year survival rate?
a. Stage I: 90% 5-year survival
b. Stage II: 45% 5-year survival
c. Stage III: 15% 5-year survival
d. Stage II: 15% 5-year survival
e. Stage III: 2% 5-year survival
Answer: b
121. Which of the following conditions is considered to increase the risk of gastric cancer?
a. Pernicious anemia
b. Prior partial gastrectomy
c. Gastric hyperplastic polyps
d. Gastric adenomatous polyps
Answer: a, b, d
122. A 55-year-old male is evaluated because of symptoms of epigastric pain and anorexia. Physical examination is normal except for guaiac positivity of stool. Upper endoscopic examination reveals a 1.5 cm ulcer along the lesser curvature of the stomach proximal to the incisura angularis. Optimal management consists of which of the following:
a. Sucralfate 1 gm q.i.d. for 8 weeks
b. Endoscopic biopsy of the ulcer rim
c. Endoscopic cautery of the ulcer base
d. Endoscopic biopsy of the ulcer base
e. Misoprostol 400 mg b.i.d. for 8 weeks
Answer: b
123. Which of the following statement(s) regarding gastric leiomyosarcoma is/are correct?
a. Leiomyosarcomas occur with peak frequency in the 2nd and 3rd decades
b. The primary histological indicator of aggressive behavior is the number of mitoses per microscopic field
c. Leiomyosarcomas are usually radiosensitive
d. Lymphadectomy is not indicated during resection because metastases are usually hematogenous
Answer: b, d